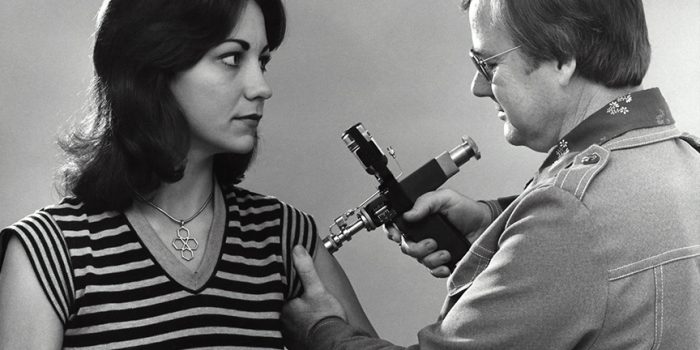
Vaccination day is a Basic Training memory that many of us in the military share—lined up with hundreds of other nervous recruits, sleep-deprived and culture-shocked, waiting to be vaccinated against who knows what. Most of us didn’t care. We had already learned that questioning orders was not a good plan.
Vaccinating recruits with air gun injection was quick and efficient. No pesky needles were necessary—just a super-fast puff of air that magically inserted vaccines right into your arm. Many people didn’t feel a thing, but there were those lucky ones who ended up with a trail of blood down their arms after unfortunately flinching.
We knew the practice was odd and made for good storytelling. But we never imagined that the government was putting us in danger of contracting a blood-borne illness like Hepatitis C.
More than five percent of veterans have Hepatitis C, and that’s three times more than those who haven’t served in the military. And studies have shown the culprit could be those air gun injectors used to vaccinate service members in mass.
History of Air Gun Injector Use in the Military
The military used air gun injectors to vaccinate millions of service members from the 1950s through the 1990s. Due to their efficiency, boasting 1,000 injections per hour, air gun injectors were a preferred method of vaccination not only in the military but through global immunization campaigns. Vaccines are delivered through the skin using a high-pressure stream of air. If the patient or vaccine administrator moved, the stream of air might rip the skin.
The Department of Defense stopped using this method in 1998 after a Hepatitis B outbreak in a California weight loss clinic was blamed on air injector use. How could this be possible? Air injectors were not cleaned between uses. Initial reports were that contamination was highly unlikely, and cleaning between each patient would slow down the process.
What is Hepatitis C?
Hepatitis C is an infection that damages the liver over time, resulting in liver cancer, cirrhosis of the liver, and potentially death. Initial symptoms are mild and often go unnoticed. In some cases, people feel no symptoms for 20 to 30 years after exposure. Some symptoms are fatigue, joint pain, and abdominal pain.
Hepatitis C is transmitted through blood contact. Common contraction methods include sharing needles, unclean injection practices, accidental needle prick, mother-to-child transmission, and sexual contact.
Since the infection is progressive, catching it early is critical to preventing deadly damage. There are several treatment options available that many times result in a full recovery.
How is Hep C Affecting Veterans?
As mentioned above, veterans are infected with Hepatitis C at a rate of five times more than the general population. One possible explanation for the increased risk is due to unsafe air gun injections during mass vaccinations.
While the VA offers testing and treatment of Hepatitis C, they are slow to recognize it as a service-connected disability which affects the veteran’s ability to receive disability compensation. It’s hard to prove the service connection for Hepatitis C since the illness goes undetected for so many years. And the longer time passes, the harder it is to pinpoint contraction.
Hepatitis C is most prevalent in Vietnam vets; in fact, 1 in 5 test positive for the infection. Air guns were at their peak use during this era. Other identified service-connected transmission methods appear on HCVet.com, a website dedicated to education and support for veterans with Hepatitis C. They are:
· Medical procedures
· Dental procedures
· Blood products
· Injection equipment
· Shared personal items (such as razors)
Medical experts at Valor 4 Vets determined that it is “as least as likely as not” that Hepatitis C is contracted from air gun injectors after several medical reviews. Yet veterans continue to have difficulty getting VA approval for service-connected disability claims. One successful appeal to note happened in 2016. The veteran served from 1975-77 and tested positive for Hepatitis C in 2007. He submitted a claim in 2008. The VA denied the claim, and he met before the appeals board in 2016.
The veteran listed two risk factors, air gun injection and sharing razors in unclean environments. Submitted evidence corroborated his statement that he never identified any other risk factors. Since there was no evidence that he had any other risk factors, the “benefit of the doubt” rule was enacted. Meaning, if there is no strong evidence one way or the other, the benefit of the doubt is given to the claimant. The VA approved his appeal.
Do You Have More Questions About Hepatitis C?
If you think there is a possibility that you have been exposed to Hepatitis C, you should get tested. A simple blood test identifies the infection, and you can get it through your primary care physician or your local VA.
Being tested now can help prevent further damage to the liver, and treatments can cure the infection. The VA has taken aggressive steps to identify and treat Hepatitis C in the veteran community and say 100,000 veterans are Hepatitis free since 2014. You can read more about the VA’s research here.
Although there have been great strides in acceptance by the VA of Hepatitis C as a service-connected disability, the VA reviews each claim individually, and decisions may differ. If you need help processing a claim or appeal to prove a service connection for Hepatitis C, our medical experts at Valor 4 Vet can help.